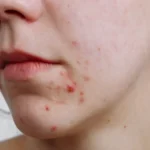
Breakouts that cluster around the mouth and chin area are one of the most common yet frequently misunderstood skin concerns. Whether you experience the occasional blemish or a persistent pattern of inflamed spots, understanding why they occur is the first step towards clearer, calmer skin.
What Is Perioral Acne?
Acne that forms around the mouth, along the chin, and at the corners of the lips is commonly referred to as perioral acne. The word perioral simply means “around the mouth,” and this localised pattern of breakouts is distinct from the kind of widespread facial acne that affects the forehead or cheeks equally.
This type of acne can present in many forms, including blackheads, whiteheads, papules, pustules, and deeper cystic nodules. It tends to be particularly stubborn, partly because the skin in this area is sensitive and partly because the triggers behind it are often ongoing rather than isolated incidents.
Understanding perioral acne requires looking at the unique characteristics of the skin in this region, as well as the many internal and external factors that can disrupt it.
Common Causes of Acne Around the Mouth
There is rarely a single explanation for why breakouts appear in this area. Most cases are driven by a combination of factors that interact with one another over time.
Hormonal fluctuations: The chin and jaw area is particularly responsive to androgens and hormonal shifts during the menstrual cycle.
Product irritation: Lip balms, toothpastes, and certain skincare products can clog pores or trigger inflammation.
Stress: Elevated cortisol increases sebum production, which can trigger or worsen breakouts in this region.
Diet and gut health: High glycaemic foods and dairy have been linked to increased acne activity in some individuals.
Touching the face: Resting hands near the mouth transfers bacteria and oils that can block follicles.
Medications: Certain steroid inhalers, corticosteroids, and contraceptives can influence breakout patterns.
Hormonal acne and the chin zone
Of all the contributing factors, hormonal activity is the one most closely associated with persistent acne around the mouth and chin. The sebaceous glands in this lower portion of the face contain a high concentration of androgen receptors. When levels of testosterone or DHEA fluctuate, as they commonly do around ovulation, menstruation, or periods of chronic stress, these receptors trigger increased oil production, which can lead to congested pores and inflammation.
Women are significantly more likely than men to experience this lower face breakout pattern. It often follows a predictable monthly rhythm, appearing or worsening in the days before or during a period. If you notice your breakouts following a cyclical pattern, hormonal influences are very likely involved.
The role of toothpaste and lip products
One of the more surprising contributors to perioral breakouts is the everyday products that come into contact with this area. Sodium lauryl sulphate, a foaming agent found in many toothpastes, can be irritating to the skin around the mouth and has been linked to both acne and perioral dermatitis in susceptible individuals. Similarly, heavily fragranced or waxy lip balms can block the small follicles along the lip border.
If your breakouts tend to cluster very close to the lips or at the corners of the mouth, it is worth reviewing your oral care products as well as any lip products you use regularly.

Acne Around the Mouth vs. Perioral Dermatitis
It is important to distinguish between standard acne and a condition called perioral dermatitis, as they can look similar but require very different approaches to treatment.
Clinical note: Perioral dermatitis typically presents as small, red, bumpy papules and pustules grouped around the mouth, nose, and sometimes the eyes. Unlike conventional acne, it rarely involves blackheads and is often accompanied by mild burning or itching. It is more common in women aged 20 to 45 and is frequently triggered or worsened by topical steroid creams, fluorinated toothpastes, and rich moisturisers.
Standard acne around the mouth, by contrast, involves the full range of comedonal and inflammatory lesions and tends to respond well to conventional acne treatments. If your breakouts look unusually uniform, feel irritated rather than simply inflamed, and you have been using steroid creams on your face, it is worth consulting a dermatologist or skin clinic before beginning treatment, as using the wrong approach can aggravate perioral dermatitis significantly.
How to Treat Acne Around the Mouth
Effective treatment depends on identifying the primary drivers of your breakouts, as a one-size-fits-all approach rarely delivers lasting results. That said, there are several well-evidenced strategies that work for the majority of people.
Topical treatments
The following active ingredients have good clinical evidence behind them for treating acne in this area:
- Benzoyl peroxide kills the bacteria responsible for inflammatory acne lesions. A low concentration formulation (2.5 to 5 percent) applied as a leave-on gel is often sufficient and causes less irritation than higher strengths.
- Salicylic acid is a beta hydroxy acid that exfoliates inside the pore, helping to break down the debris that causes blackheads and whiteheads. It is particularly useful for congested, non-inflammatory breakouts.
- Azelaic acid has antibacterial, anti-inflammatory, and mild keratolytic properties. It is gentler than benzoyl peroxide and retinoids, making it a good option for sensitive skin or darker skin tones where post-inflammatory hyperpigmentation is a concern.
- Topical retinoids such as adapalene normalise the rate of skin cell turnover inside the follicle, preventing the buildup that leads to comedones. They require consistent use over several weeks before results become visible.
- Niacinamide helps regulate sebum production, calm inflammation, and strengthen the skin barrier. Whilst it is not a standalone treatment for active acne, it works well alongside other actives.
Important: Apply topical actives carefully around the lip border. The skin immediately at the edge of the lips is thinner and more reactive, and over-application of strong treatments can cause dryness, peeling, and irritation that makes the area look worse before it improves.
Hormonal treatments
If your acne is primarily driven by hormonal fluctuations, topical treatments alone may produce limited results. A GP or dermatologist can assess whether hormonal therapy is appropriate. Options include combined oral contraceptive pills with anti-androgenic activity, such as those containing cyproterone acetate or drospirenone, or the medication spironolactone, which reduces androgen activity in the skin.
These options are particularly worth exploring if your breakouts are cystic, follow a clear monthly pattern, or have not responded well to multiple topical treatments over a consistent period.
Professional clinic treatments
In-clinic treatments can make a significant difference, particularly for persistent or inflammatory acne that has not responded well to over-the-counter options. Treatments that are commonly used for perioral acne include chemical peels using salicylic acid or glycolic acid, light-based therapies such as blue LED or photodynamic therapy, and microneedling with targeted serums to address both active breakouts and the scarring or pigmentation they can leave behind.
A qualified skin clinician will be able to assess your skin thoroughly and recommend a treatment plan tailored to your specific pattern of acne, skin type, and any contributing lifestyle factors.
Skincare Habits That Support Clearer Skin
Beyond active treatments, establishing a consistent and appropriate skincare routine is essential for managing perioral acne over the long term.
Cleansing: Use a gentle, non-stripping cleanser twice daily. Avoid anything heavily fragranced or formulated with sulphates. Thorough but gentle cleansing removes the toothpaste, food residue, and product buildup that can accumulate around the mouth area throughout the day.
Moisturising: A common misconception is that oily or acne-prone skin does not need moisturiser. An intact skin barrier actually helps regulate sebum production and reduces the irritation that makes acne worse. Choose a lightweight, non-comedogenic moisturiser and apply it consistently, even when using drying actives such as benzoyl peroxide.
Sun protection: Daily SPF is non-negotiable, particularly when using retinoids or chemical exfoliants that increase photosensitivity. Post-inflammatory hyperpigmentation, the dark marks that acne spots leave behind, becomes significantly more pronounced with unprotected sun exposure. Choose an SPF formulation that is labelled non-comedogenic or oil-free.
Practical tip: Review your lip balm ingredients and consider switching to a fragrance-free, non-comedogenic formula. If you use a steroid inhaler, rinse your face gently after use, as any residue around the mouth can disrupt the local skin microbiome and trigger breakouts.
Lifestyle Factors Worth Considering
Skin health is rarely isolated from overall wellbeing. Several lifestyle factors have a documented influence on acne activity and are worth addressing alongside any topical or medical treatment programme.
Diet and blood sugar balance
A growing body of research supports a link between high glycaemic index diets and increased acne severity. Foods that cause rapid spikes in blood sugar stimulate insulin and insulin-like growth factor 1 (IGF-1), both of which promote sebum production and increase the likelihood of blocked pores. Reducing refined carbohydrates and sugar whilst increasing fibre, vegetables, and protein may have a noticeable effect on breakout frequency for some individuals.
The evidence for dairy, particularly skimmed milk, is also reasonably consistent, though responses vary. Keeping a food diary alongside a breakout log can help identify whether specific foods appear to correlate with flares.
Stress management
Psychological stress elevates cortisol, which in turn increases androgen activity and sebum production. It also disrupts the gut microbiome and can lead to poor sleep, both of which have secondary effects on skin health. Whilst eliminating stress entirely is not realistic, practices such as regular physical activity, adequate sleep, and techniques like mindfulness or breathwork can meaningfully reduce its impact on the skin over time.
Gut health
The gut-skin axis is an area of growing interest in dermatology. The diversity and health of the gut microbiome appears to influence systemic inflammation, which in turn affects the skin. Probiotic-rich foods, adequate fibre intake, and limiting ultra-processed foods may support clearer skin as part of a broader approach to health.
When to Seek Professional Advice
Mild to moderate perioral acne can often be managed effectively with the right combination of over-the-counter treatments and consistent skincare habits. However, there are circumstances in which professional input is clearly advisable.
Seek professional advice if your acne is cystic or nodular, if it has not improved after two to three months of consistent topical treatment, if it is leaving significant scarring or hyperpigmentation, if you suspect a hormonal underlying cause, or if you are unsure whether you are dealing with acne or perioral dermatitis.
A skin clinic or dermatologist can provide a thorough assessment, rule out other conditions, and create a treatment plan with access to prescription-strength options that are not available over the counter. Early professional intervention can prevent the cycle of recurring breakouts and the cumulative skin damage they cause.
Frequently Asked Questions
Can acne around the mouth be caused by my toothpaste?
Yes, in some cases. Sodium lauryl sulphate, fluoride, and flavouring agents in certain toothpastes can irritate the skin around the mouth and trigger or worsen breakouts. Try switching to a fluoride-free, sulphate-free formulation for several weeks to assess whether it makes a difference. Rinsing your face after brushing your teeth is also a sensible habit.
Why do my breakouts always come back in the same place?
Recurring breakouts in the same area typically indicate an ongoing trigger rather than a single isolated event. For the perioral region, this is most often hormonal fluctuation, a product interaction, or habitual skin touching. Identifying and addressing the root cause, rather than simply treating each breakout as it appears, is the most effective long-term strategy.
Are perioral breakouts always acne?
Not always. Perioral dermatitis, folliculitis, contact dermatitis, and cold sore outbreaks can all be mistaken for acne in this area. If your breakouts look atypical, are accompanied by burning or itching, or are not responding to standard acne treatments, a professional assessment is worthwhile.
How long will it take to see improvement?
Most topical treatments require a minimum of eight to twelve weeks of consistent use before results become apparent. Hormonal treatments typically take three to six months to show their full benefit. Patience and consistency are essential. Beginning multiple new treatments simultaneously also makes it difficult to identify what is working, so introducing changes one at a time is generally advisable.
Acne around the mouth is common, often frustrating, and highly treatable. With the right understanding of what is driving your breakouts and a consistent, appropriately targeted approach to treatment, significant and lasting improvement is absolutely achievable. If you would like personalised guidance, the team at Linia Skin Clinic is available to help with a comprehensive skin consultation tailored to your specific needs.