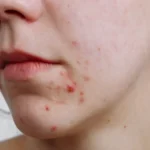
What Is Menopausal Acne?
Menopausal acne refers to acne that develops, or significantly worsens, during perimenopause, menopause, or the postmenopausal period. It is a subtype of adult hormonal acne, and its root cause lies in the dramatic hormonal shifts that characterise the menopausal transition.
Unlike teenage acne, which is typically driven by a general surge of sex hormones across the board, menopausal acne arises from a specific hormonal imbalance: the steep decline of oestrogen and progesterone whilst androgens (male sex hormones such as testosterone) decline at a comparatively slower pace. This creates what clinicians refer to as relative androgen dominance, a state in which the skin becomes disproportionately sensitive to androgenic stimulation, resulting in increased sebum production, clogged pores, and inflammatory breakouts.
Crucially, this form of acne can appear for the very first time in a woman’s life during the menopausal transition, even in those with no prior history of problematic skin. Equally common is a recurrence or escalation of acne in women who previously experienced hormonal breakouts in their teens or around their menstrual cycle.
The Three Hormonal Phases and Their Impact on the Skin
The menopausal transition does not happen overnight. Understanding the distinct hormonal phases helps clarify why skin changes can begin years before menopause is officially reached.
- Perimenopause (Typically Ages 40–51): This transitional phase can begin up to ten years before menopause itself and is marked by irregular, fluctuating levels of oestrogen and progesterone. The unpredictability of hormone levels during this period is particularly acne provocative, as the skin’s oil glands receive inconsistent signalling, often resulting in cyclical breakouts that do not correspond neatly to the menstrual cycle. Many women first notice menopausal acne during this phase, often misattributing it to stress or diet.
- Menopause (Confirmed After 12 Consecutive Months Without Menstruation): At menopause, oestrogen and progesterone levels fall significantly and more consistently. Testosterone, produced in smaller amounts by the ovaries and adrenal glands, declines too, but far more gradually. This hormonal imbalance favours androgenic skin activity: increased sebum production, heightened follicular inflammation, and a slower rate of skin cell turnover, all of which combine to perpetuate breakouts.
- Postmenopause: For some women, acne resolves as hormone levels stabilise at their new, lower baseline. For others, particularly those with a genetic predisposition to adult acne or elevated adrenal androgen production, breakouts can persist into the postmenopausal years. In these cases, additional investigation may be warranted to rule out underlying conditions such as polycystic ovary syndrome (PCOS), adrenal hyperplasia, or thyroid dysfunction.
The Biology Behind Menopausal Breakouts
To understand menopausal acne fully, it is necessary to look at how oestrogen influences the skin under normal circumstances, and what is lost when its levels fall.
Oestrogen has profound anti-inflammatory, collagen-stimulating, and sebum-regulating effects on the skin. It binds to oestrogen receptors found abundantly in skin cells, hair follicles, and sebaceous (oil) glands, where it moderates the skin’s response to androgens. When oestrogen is plentiful, testosterone’s stimulating effect on sebaceous glands is effectively buffered. When oestrogen declines, that buffer is removed.
Androgens, including testosterone and DHEA-S (dehydroepiandrosterone sulphate), produced by the adrenal glands, bind to androgen receptors in the sebaceous glands and stimulate the production of sebum. In the absence of adequate oestrogen, this stimulation goes partially unchecked, leading to excess sebum, follicular blockage, and the proliferation of Cutibacterium acnes, the bacteria responsible for inflammatory acne lesions.
Additionally, oestrogen normally promotes keratinocyte (skin cell) differentiation and turnover. When oestrogen falls, skin cell shedding slows, increasing the likelihood that dead skin cells will accumulate within follicles and contribute to comedone formation.
⚗️: Relative Androgen Dominance
Testosterone’s influence on sebaceous glands becomes more pronounced as oestrogen declines, driving excess oil production even without a rise in absolute androgen levels.
🔬: Slower Cell Turnover
Reduced oestrogen slows the shedding of skin cells, increasing the risk of follicular blockage and comedone formation, the foundation of all acne lesions.
🌡️: Cortisol and Stress
Hot flushes, night sweats, insomnia, and the psychological demands of the menopause transition elevate cortisol levels, a stress hormone that directly stimulates androgen production and worsens acne.
💧: Skin Barrier Changes
Lower oestrogen reduces ceramide production, compromising the skin’s protective barrier and making it simultaneously more prone to dehydration and inflammatory reactions.
How Menopausal Acne Looks and Where It Appears
Recognising menopausal acne is an important step in ensuring it receives appropriate treatment rather than being managed with products designed for teenage skin, an approach that frequently makes matters worse.
| Feature | Menopausal Acne | Teenage Acne |
|---|---|---|
| Primary location | KeyLower face, jawline, chin, neck | Forehead, nose, cheeks (T-zone) |
| Predominant lesion type | Deep, inflammatory cysts and nodules; some comedones | Whiteheads, blackheads, pustules across broader areas |
| Skin context | KeyOccurs alongside dry, thinning, or combination skin | Typically occurs on oilier, more resilient skin |
| Scarring potential | Higher — mature skin heals more slowly, increasing PIH and structural scarring risk | Present, but skin regenerates more rapidly |
| Cyclical pattern | May lack clear cycle link during perimenopause; often persistent | Frequently worsens before menstruation |
| Associated changes | Hot flushes, night sweats, mood changes, sleep disruption, vaginal dryness | Growth spurts, general hormonal surges |
Factors That Worsen Menopausal Acne
Whilst hormonal changes are the primary driver, several additional factors can significantly exacerbate menopausal acne. Understanding and addressing these can meaningfully reduce breakout frequency and severity, particularly when hormonal treatment is not immediately appropriate or desired.
Sleep Deprivation
Poor sleep, frequently caused by night sweats and insomnia associated with the menopause transition, raises cortisol levels and impairs the overnight skin repair process. Research indicates that elevated cortisol promotes androgen synthesis, which in turn worsens acne. Additionally, growth hormone, which supports skin renewal, is released predominantly during deep sleep; its disruption accelerates skin ageing and slows post-breakout healing.
Diet and Blood Sugar Fluctuations
High-glycaemic foods, including refined sugars, white bread, white rice, and processed snacks, cause rapid spikes in blood glucose and insulin levels. Elevated insulin stimulates androgen production and increases the availability of insulin-like growth factor 1 (IGF-1), both of which drive sebum synthesis and acne activity. Emerging evidence also links high consumption of skimmed milk to worsening acne, potentially due to the presence of hormonal precursors in dairy products.
Hormone Replacement Therapy (HRT)
Whilst HRT is often considered a first-line approach for managing menopausal symptoms, certain formulations, particularly those containing synthetic progestins, may exacerbate acne in susceptible individuals. Progestins with androgenic activity, such as some older formulations of norethisterone, can stimulate sebaceous gland activity. Conversely, HRT formulations using oestradiol combined with body-identical progesterone, rather than synthetic progestin, may be more skin-friendly and, in some cases, can actually improve acne. This highlights the importance of discussing skin outcomes specifically with a prescribing doctor when initiating HRT.
Comedogenic Skincare and Cosmetics
Products containing pore-blocking, comedogenic ingredients, including certain silicones, heavy mineral oils, and cocoa butter in large quantities, can worsen congestion in already-compromised follicles. During the menopause transition, when skin may feel drier and more sensitive, there is a natural temptation to use richer, more emollient products. Care must be taken to choose formulations that are both deeply moisturising and non-comedogenic.
Important: If menopausal acne is severe, sudden in onset, accompanied by signs of virilisation, such as notable facial hair growth, deepening voice, or hair loss, or fails to respond to standard treatment, a medical evaluation is strongly recommended. In rare cases, sudden or severe androgenic changes can indicate an underlying ovarian or adrenal condition requiring investigation.

Professional Treatments for Menopausal Acne
Managing menopausal acne effectively often requires a combination of approaches: addressing the hormonal root cause, treating existing acne lesions, and repairing any skin damage already caused. The following treatments have demonstrated clinical efficacy and can be tailored to the unique needs of mature skin.
#First-Line Hormonal
Spironolactone
An androgen-blocking medication traditionally used as a diuretic, spironolactone has become a cornerstone treatment for adult hormonal acne in women. At low doses (50–150mg daily), it reduces the effect of androgens on sebaceous glands, significantly decreasing sebum production. It is generally well tolerated, though it requires regular monitoring and is contraindicated in pregnancy. It is considered the first-choice oral anti-androgen therapy for menopausal acne in the UK when topical treatments alone are insufficient.
#Hormonal Support
Hormone Replacement Therapy (HRT)
When formulated appropriately, HRT can address menopausal acne by restoring some degree of the skin’s oestrogenic environment and reducing the relative androgen dominance driving breakouts. Body-identical oestradiol combined with micronised progesterone (rather than androgenic synthetic progestins) is generally the preferred formulation for skin-conscious patients. HRT should always be initiated and monitored by a qualified prescriber, with skin outcomes discussed as part of the overall treatment plan.
#Topical Prescription
Retinoids (Tretinoin / Adapalene)
Retinoids are vitamin A derivatives that accelerate skin cell turnover, prevent follicular blockage, and stimulate collagen production, addressing both active acne and the signs of skin ageing simultaneously. Prescription tretinoin is more potent than over-the-counter retinol and is often the topical treatment of choice for menopausal acne alongside a comprehensive skincare routine. Because mature skin is more susceptible to irritation, a low concentration introduced gradually is essential.
#Oral Antibiotic
Short-Course Antibiotics
For moderate inflammatory menopausal acne, a limited course of oral antibiotics (such as doxycycline or lymecycline) can reduce the bacterial load and break the inflammatory cycle whilst longer-term strategies take effect. Due to concerns regarding antibiotic resistance, these are rarely prescribed as a standalone solution, but can be effective as a short-term bridge treatment.
#Clinic Treatment
RF Microneedling
Radiofrequency microneedling delivers controlled energy to the dermis via fine insulated needles, stimulating collagen and elastin production whilst simultaneously reducing sebaceous gland activity. It is particularly beneficial for menopausal acne as it addresses active breakouts, post-acne scarring, and the skin laxity associated with oestrogen decline, all in a single treatment modality with minimal downtime.
#Clinic Treatment
Chemical Peels
Superficial-to-medium chemical peels using salicylic acid, lactic acid, or mandelic acid can effectively decongest pores, accelerate cell turnover, and reduce post-inflammatory pigmentation. For mature skin, gentler acids (such as lactic or mandelic) are often better tolerated than glycolic acid at equivalent concentrations, providing meaningful exfoliation without compromising a skin barrier that is already less robust due to oestrogen deficiency.
A Skincare Routine for Menopausal Acne-Prone Skin
Menopausal skin requires a careful balance: effective acne management without the harshness that can compromise a fragile skin barrier. The following protocol reflects best practice for this unique skin profile.
Morning Routine
Gentle, non-foaming cleanser: Avoid soap-based cleansers that strip the skin’s natural oils. Look for pH-balanced, fragrance-free formulations containing mild surfactants such as coco-glucoside.
Niacinamide serum (4–10%): Reduces sebum production, calms inflammation, and helps maintain the skin barrier without aggravating acne-prone follicles.
Vitamin C serum (10–15% L-ascorbic acid): Antioxidant protection, collagen support, and assistance fading any post-acne hyperpigmentation. Apply before moisturiser.
Non-comedogenic, lightweight moisturiser: Ceramide- or hyaluronic acid-based formulations replenish the skin barrier without blocking pores. Essential even in acne-prone skin.
Broad-spectrum SPF 30+ (non-comedogenic): Mandatory every day. UV exposure stimulates melanin production, deepening any existing dark marks left by acne.
Evening Routine
Double cleanse (if wearing SPF or makeup): Begin with a micellar water or gentle cleansing oil to remove sunscreen and makeup, followed by the same gentle cleanser used in the morning.
Retinoid (retinol or tretinoin): Applied two to three evenings per week initially, increasing frequency as tolerated. Promotes cell turnover, prevents comedone formation, and supports collagen production.
Targeted acne spot treatment: On non-retinoid nights, apply a salicylic acid or benzoyl peroxide spot treatment directly to active lesions. Avoid applying across the entire face to prevent excessive dryness.
Richer moisturiser with barrier-supporting ingredients: Ceramides, squalane, and panthenol are particularly beneficial for repairing and maintaining a compromised barrier overnight. Use a slightly richer formulation than in the morning.
Optional: azelaic acid (on alternate evenings): If post-inflammatory hyperpigmentation is a concern, azelaic acid is a gentle, effective brightening agent safe for long-term use in mature skin.
10 Expert Tips for Managing Menopausal Acne
Evidence-based guidance from our specialist team, designed specifically for the complexities of hormonal acne in mature skin.
- Seek a Specialist Assessment Early: Menopausal acne has a hormonal root cause that over-the-counter acne products alone are rarely equipped to address comprehensively. The sooner you consult a dermatologist or aesthetic medicine specialist with experience in adult hormonal acne, the sooner an appropriate treatment plan, which may include prescription topicals, anti-androgen therapy, or clinic procedures, can be put in place. Early intervention significantly reduces the risk of post-inflammatory scarring, which is harder to treat in mature skin.
- Avoid Harsh, Drying Acne Products Designed for Teenage Skin: Products formulated for teenage acne, particularly those containing high concentrations of benzoyl peroxide, alcohol-heavy toners, or aggressive exfoliants, can seriously compromise the already-reduced skin barrier of menopausal skin. Stripping the skin’s natural oils triggers a compensatory sebum surge, known as reactive seborrhoea, potentially worsening breakouts. Stick to clinically validated ingredients at concentrations appropriate for mature skin, and always pair active ingredients with adequate moisturisation.
- Switch to a Low-Glycaemic Diet: Reducing the glycaemic load of your diet is one of the most impactful lifestyle changes you can make for menopausal acne. Replace refined carbohydrates and sugary foods with complex carbohydrates, such as oats, legumes, and wholegrain foods, lean protein, and anti-inflammatory fats, particularly omega-3 fatty acids found in oily fish, walnuts, and flaxseeds. Emerging evidence supports the inclusion of phytoestrogen-rich foods, such as soy products, flaxseeds, and chickpeas, as a means of gently supporting hormonal balance during the menopausal transition.
- Prioritise Sleep and Address Night Sweats Proactively: Poor sleep is both a consequence of menopause and a significant driver of worsened acne. Elevated cortisol from chronic sleep deprivation promotes androgen synthesis and increases skin inflammation. If night sweats are disrupting your sleep, speak to your GP or menopause specialist about management strategies, including HRT, CBT-based approaches, or non-hormonal medications. Even modest improvements in sleep quality can have a measurable positive impact on hormonal acne
- Introduce a Retinoid Into Your Evening Routine: Retinoids are arguably the most versatile topical ingredients available for menopausal acne-prone skin, simultaneously addressing active breakouts, post-acne hyperpigmentation, and the collagen loss that accelerates during the menopausal transition. Begin with a low-concentration retinol (0.1–0.3%) or over-the-counter adapalene, applied every other evening on a buffered basis, applying moisturiser first, then retinoid on top. Increase frequency gradually as your skin builds tolerance. Those with more significant acne may benefit from prescription-strength tretinoin, which should be initiated under clinical guidance.
- Ask Your Doctor About Spironolactone: For women whose menopausal acne does not respond adequately to topical treatments, spironolactone, an oral anti-androgen medication, is frequently the most effective next step. By blocking the effect of testosterone on sebaceous glands, it addresses the fundamental hormonal driver of breakouts rather than simply treating their surface manifestations. It is generally well tolerated, though it is not appropriate for all individuals and requires a medical assessment before prescribing. Discuss this option with your GP, gynaecologist, or dermatologist.
- Manage Stress Consistently and Intentionally: Chronic stress is one of the most underestimated drivers of menopausal acne. Cortisol, the primary stress hormone, directly stimulates the adrenal glands to produce androgens, compounding the hormonal imbalance already present during menopause. Regular physical activity, mindfulness practices, breathing techniques, and adequate social connection are all clinically supported approaches to cortisol regulation. Whilst eliminating stress entirely is unrealistic, developing a consistent stress management practice can meaningfully reduce breakout frequency and severity.
- Audit Your HRT Formulation if Applicable: If you are taking hormone replacement therapy and have noticed that your acne developed or worsened after starting it, the progestin component of your HRT may be contributory. Older synthetic progestins with androgenic activity can stimulate sebum production. Discussing a switch to a formulation containing body-identical, micronised progesterone, which has a more neutral skin profile, may be worthwhile. This conversation should take place with your prescribing doctor and should not lead to an abrupt cessation of HRT without medical guidance.
- Wear SPF Every Day Without Exception: Daily sun protection is non-negotiable for anyone managing menopausal acne. UV exposure worsens post-inflammatory hyperpigmentation, the dark marks left behind after acne lesions heal, and this pigmentation tends to be more persistent in mature skin due to slower cell turnover. Additionally, UV radiation stimulates melanocyte activity and degrades collagen, accelerating the visible signs of skin ageing. Choose a broad-spectrum mineral or hybrid SPF 30+ formulation that is non-comedogenic and does not feel heavy on the skin.
- Stay Consistent and Be Realistic About Timelines: Menopausal acne, driven as it is by hormonal changes that cannot be reversed overnight, requires patience and consistency. Even with the right topical products, oral treatments, and lifestyle adjustments in place, meaningful improvement typically takes between eight and sixteen weeks. The temptation to switch products frequently or abandon a regimen before it has had adequate time to work is one of the most common barriers to successful outcomes. Document your skin with monthly photographs, maintain your routine, and communicate regularly with your treating clinician so that adjustments can be made as needed based on evidence rather than impatience.
Key Ingredients for Menopausal Acne-Prone Skin
When selecting skincare products for menopausal acne-prone skin, look for the following clinically validated ingredients. Prioritise formulations that are fragrance-free, non-comedogenic, and designed for sensitive or mature skin.
#Exfoliant · Acne
Salicylic Acid
Oil-soluble BHA that penetrates pores to dissolve congestion. Safe and effective at 0.5–2% for clearing menopausal breakouts without excessive dryness.
#Cell Turnover
Retinoids
Tretinoin, adapalene, or retinol accelerate cell renewal, prevent comedones, and stimulate collagen — addressing acne and ageing simultaneously.
#Multi-benefit
Niacinamide
Regulates sebum, strengthens the skin barrier, reduces inflammation, and fades hyperpigmentation. Exceptionally well tolerated in mature skin.
#Brightening
Azelaic Acid
Antimicrobial, anti-inflammatory, and melanin-inhibiting. Ideal for treating both active menopausal acne and the PIH it leaves behind.
#Antioxidant
Vitamin C
L-ascorbic acid supports collagen synthesis, brightens hyperpigmentation, and offers antioxidant protection against UV-induced skin damage.
#Hydration
Hyaluronic Acid
Draws and retains moisture in the skin. Essential for maintaining hydration in menopausal skin without adding pore-blocking oils.
#Barrier Repair
Ceramides
Replenish the skin’s lipid barrier, reducing transepidermal water loss and the inflammatory sensitivity that underlies menopausal acne flares.
#Pigmentation
Tranexamic Acid
Inhibits melanin-triggering pathways, making it highly effective for stubborn post-acne dark marks in post-menopausal skin.
When to Seek Urgent Medical Advice
Whilst menopausal acne is common and generally manageable, certain presentations warrant prompt medical evaluation. If your acne is severe or rapidly worsening, if you notice signs of virilisation (significant facial hair growth, voice changes, hair thinning), if breakouts are accompanied by significant menstrual irregularity or pelvic pain, or if standard treatments consistently fail to provide relief, please consult your GP or a specialist. These symptoms may indicate an underlying hormonal condition such as PCOS, adrenal hyperplasia, or, rarely, an androgen-secreting tumour.