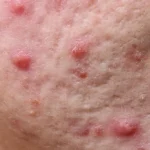
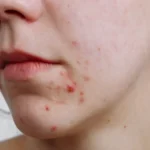
Acne is one of the most common skin conditions affecting people of all ages and backgrounds. While many consider acne as simply “breakouts,” understanding the specific type of acne you’re experiencing is crucial for effective treatment. Two of the most prevalent forms—bacterial acne and hormonal acne—require different approaches for optimal results.
At Linia Skin Clinic, we believe informed patients make better decisions about their skin health. This comprehensive guide will help you distinguish between bacterial and hormonal acne, understand their unique causes, recognize their distinctive characteristics, and discover the most effective treatment strategies for each.

Understanding Bacterial Acne
The Microbial Culprit
Bacterial acne develops primarily due to the overgrowth of Cutibacterium acnes (formerly known as Propionibacterium acnes or P. acnes), a naturally occurring bacterium that resides on our skin. Under normal circumstances, these bacteria are harmless and even beneficial. However, when certain conditions arise—such as excess oil production and clogged pores—these bacteria multiply rapidly, leading to inflammation and the formation of acne lesions.
Key Causes and Triggers of Bacterial Acne
- Excess Sebum Production: When sebaceous glands produce too much oil, pores become clogged, creating the perfect environment for bacterial growth.
- Accumulation of Dead Skin Cells: If skin cells don’t shed properly, they can combine with sebum to block follicles, trapping bacteria beneath the skin’s surface.
- Inflammatory Response: As bacteria multiply, your immune system triggers an inflammatory response, resulting in the redness and swelling characteristic of acne lesions.
- Environmental Factors: External elements like humidity, pollution, and certain cosmetic products can exacerbate bacterial acne by introducing additional bacteria or clogging pores.
- Inadequate Cleansing: While acne isn’t caused by poor hygiene, insufficient cleansing can allow oil, debris, and bacteria to accumulate, potentially worsening existing acne.
Decoding Hormonal Acne
The Hormonal Connection
Hormonal acne, as the name suggests, is directly influenced by fluctuations in hormone levels, particularly androgens (such as testosterone). These hormones stimulate the sebaceous glands to produce more oil, setting the stage for acne formation.
Primary Causes and Triggers of Hormonal Acne
- Puberty: The significant hormonal changes during adolescence lead to increased androgen production, resulting in enhanced sebum output and subsequent acne development.
- Menstrual Cycles: Many women experience predictable breakouts before or during their periods due to cyclical hormonal fluctuations.
- Polycystic Ovary Syndrome (PCOS): This condition causes elevated androgen levels, leading to persistent acne alongside other symptoms like irregular periods and excess facial hair.
- Pregnancy and Postpartum: The dramatic hormonal shifts during pregnancy and after childbirth can either improve or worsen acne, depending on individual hormonal responses.
- Menopause: Declining estrogen levels during perimenopause and menopause can lead to relative androgen dominance, triggering acne in some women.
- Stress: Chronic stress elevates cortisol levels, which can disrupt hormonal balance and potentially trigger or worsen acne.
Distinguishing Between Bacterial and Hormonal Acne
Determining whether your acne is primarily bacterial or hormonal is essential for selecting the most effective treatment approach. Here are key differences to help you identify which type you might be experiencing:
Location of Breakouts
- Bacterial Acne: Commonly appears across the forehead, nose, and cheeks (T-zone area), where oil glands are most concentrated.
- Hormonal Acne: Typically manifests along the lower third of the face—particularly the jawline, chin, and neck.
Appearance and Characteristics
- Bacterial Acne: Often presents as various types of lesions, including whiteheads, blackheads, papules, and pustules of different sizes.
- Hormonal Acne: Tends to form deeper, painful cystic lesions that may not come to a head and can take longer to resolve.
Timing and Patterns
- Bacterial Acne: Generally follows no specific timing pattern and may be consistently present.
- Hormonal Acne: Frequently follows a cyclical pattern, with flare-ups occurring at predictable times, such as before menstruation in women.
Age and Demographics
- Bacterial Acne: More prevalent during adolescence and early adulthood, affecting all genders relatively equally.
- Hormonal Acne: Can persist well into adulthood, particularly affecting women in their 20s, 30s, and even 40s.
Response to Treatment
- Bacterial Acne: Often responds well to topical treatments containing ingredients that target bacteria and reduce oil production.
- Hormonal Acne: May be resistant to conventional topical treatments and frequently requires interventions that address hormonal imbalances.
| Characteristic | Bacterial Acne | Hormonal Acne |
| Primary Location | T-zone (forehead, nose, cheeks) | Lower face (chin, jawline, neck) |
| Typical Lesions | Whiteheads, blackheads, papules, pustules | Lower face (chin, jawline, neck) |
| Pattern | No specific timing pattern | Often cyclical, related to hormonal fluctuations |
| Age Group | Primarily teens and young adults | Can persist through adulthood, especially in women |
| Associated Symptoms | Inflammation, redness, occasional discomfort | Painful lesions, potential connection to other hormonal symptoms |
| Treatment Response | Responsive to topical antibacterial agents | May require hormonal interventions |
Effective Treatment Strategies
For Bacterial Acne
- Consistent Cleansing Routine: Use a gentle, non-comedogenic cleanser twice daily to remove excess oil and debris without stripping the skin.
- Targeted Topical Treatments:
- Benzoyl peroxide (2.5-10%): Effectively kills acne-causing bacteria and helps reduce inflammation
- Salicylic acid (0.5-2%): Exfoliates within pores to prevent clogging
- Azelaic acid: Offers antibacterial and anti-inflammatory benefits with minimal irritation
- Professional Treatments:
- Prescription-strength topical antibiotics (e.g., clindamycin, erythromycin)
- Oral antibiotics for moderate to severe cases (e.g., doxycycline, minocycline)
- Chemical peels to remove dead skin cells and reduce bacterial load
- Blue light therapy to target and destroy acne-causing bacteria
- Retinoids: Topical retinoids like tretinoin or adapalene can prevent clogged pores and reduce inflammation.
For Hormonal Acne
- Hormonal Regulation:
- Oral contraceptives (for women): Certain birth control pills can help regulate hormones and reduce acne
- Anti-androgen medications (e.g., spironolactone): Help block the effects of androgens on sebaceous glands
- Dietary Considerations:
- Reducing high-glycemic foods and dairy products, which may influence hormonal activity in some individuals
- Incorporating anti-inflammatory foods rich in omega-3 fatty acids, antioxidants, and zinc
- Stress Management:
- Regular exercise, adequate sleep, and mindfulness practices to help balance hormone levels
- Yoga, meditation, or other relaxation techniques to reduce cortisol production
- Specialized Skincare:
- Products containing niacinamide, green tea extract, or botanical anti-androgens
- Oil-free, non-comedogenic moisturizers and sunscreens
- Gentle exfoliation to prevent clogged pores without triggering inflammation
- Professional Interventions:
- Cortisone injections for painful cystic lesions
- Chemical peels with salicylic or glycolic acid
- Prescription-strength retinoids to regulate cell turnover
When to Seek Professional Help
While mild acne can often be managed with over-the-counter products and consistent skincare, certain situations warrant professional dermatological care:
- Acne that doesn’t respond to over-the-counter treatments after 6-8 weeks
- Severe, painful, or cystic acne
- Acne that leaves scars or pigmentation changes
- Sudden onset of adult acne, which may indicate an underlying health issue
- Acne accompanied by other symptoms like irregular menstrual cycles or excess facial hair
Linia Skin Clinic’s Approach to Acne Treatment
At Linia Skin Clinic, we understand that acne treatment isn’t one-size-fits-all. Our approach involves:
- Comprehensive Assessment: We carefully evaluate your skin condition, medical history, lifestyle factors, and potential triggers to determine the primary type and causes of your acne.
- Customized Treatment Plans: Based on our assessment, we develop personalized treatment strategies that address your specific acne type, severity, and skin characteristics.
- Combination Therapies: For optimal results, we often recommend a multi-faceted approach that may include medical treatments, professional procedures, skincare recommendations, and lifestyle modifications.
- Ongoing Support: We provide continuous guidance and adjust treatments as needed to ensure the best possible outcomes for your skin health.
Conclusion
Understanding whether your acne is primarily bacterial or hormonal is the first step toward effective treatment. While these types can sometimes overlap or co-exist, identifying the dominant form allows for a more targeted approach.
If you’re struggling with persistent acne or are unsure about which type you’re experiencing, we invite you to schedule a consultation at Linia Skin Clinic. Our experienced dermatologists and skincare specialists can provide expert diagnosis and develop a personalized treatment plan to help you achieve clearer, healthier skin.
Remember, acne—whether bacterial or hormonal—is a medical condition, not a reflection of personal hygiene or self-care. With the right approach and professional guidance, most acne can be effectively managed, allowing you to feel confident in your skin once again.