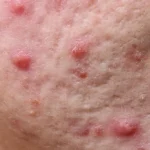
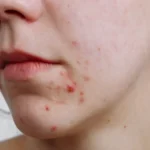
What is Acne?
Acne occurs when hair follicles become clogged with oil and dead skin cells. These blocked pores can develop into various types of blemishes on the skin’s surface. While acne most commonly appears on the face, it can also affect the back, chest, shoulders, and other areas of the body.

Common Causes of Acne
Several factors contribute to the development of acne:
Excess Oil Production: The sebaceous glands produce an oily substance called sebum. When these glands produce too much oil, it can combine with dead skin cells to block pores.
Bacteria: Propionibacterium acnes (P. acnes) is a naturally occurring bacteria that lives on the skin. When trapped in blocked pores, these bacteria can multiply rapidly, causing inflammation and infection.
Hormones: Hormonal changes, particularly during puberty, can stimulate the sebaceous glands to produce more oil. This explains why teenagers are especially prone to acne. Hormonal fluctuations during menstruation, pregnancy, or when starting or stopping birth control pills can also trigger breakouts in women.
Genetics: Your family history plays a role in your likelihood of developing acne. If your parents had acne, you’re more likely to experience it too.
Diet: Some research suggests that certain foods, particularly those with a high glycemic index (such as sugary foods and refined carbohydrates) and dairy products, may trigger or worsen acne in some people.
Stress: While stress doesn’t directly cause acne, it can exacerbate existing acne by triggering hormonal changes and inflammation.
Recognizing Acne Symptoms
Acne can manifest in several forms:
Whiteheads: Closed, clogged pores that appear as small, flesh-colored or white bumps on the skin’s surface.
Blackheads: Open, clogged pores where the trapped material is exposed to air, causing it to darken. Contrary to popular belief, the black color is not due to dirt but results from oxidation.
Papules: Small, tender red bumps that indicate inflammation or infection in the hair follicles.
Pustules: Similar to papules but containing pus at their tips, usually white or yellow in color.
Nodules: Large, solid, painful lumps beneath the skin’s surface. These develop when the infection extends deeper into the skin.
Cysts: Deep, painful, pus-filled lesions that can cause scarring. Cystic acne is the most severe form of the condition.
Risk Factors for Developing Acne
Medical researchers continue to investigate why acne affects some individuals more severely than others. However, several established risk factors have been identified:
Hormonal Changes: Times of significant hormonal fluctuation such as puberty, pregnancy, and menstrual cycles can trigger or worsen acne outbreaks.
Medical Conditions: Endocrine disorders like polycystic ovarian syndrome (PCOS) often present with acne as a symptom due to hormonal imbalances.
Lifestyle Factors: Scientific evidence suggests that cigarette smoking and inadequate sleep can contribute to acne development and severity.
Skincare Products: Beauty products containing high oil content may clog pores and exacerbate acne. Look for “non-comedogenic” labels when purchasing cosmetics and skincare items.
Medications: Certain pharmaceutical treatments including lithium, some hormonal contraceptives, anticonvulsants, and corticosteroids can trigger acne as a side effect.
Genetic Predisposition: Having parents or close relatives with acne increases your likelihood of experiencing it as well, suggesting a hereditary component.

Diet and Nutrition: Research published in 2021 indicates potential connections between diet and acne:
- Foods with high glycemic indexes (such as processed carbohydrates and added sugars) may increase acne severity
- Certain dairy products, particularly milk and ice cream, appear to worsen acne in some individuals, though cheese seems less problematic
- Omega-3 and omega-6 fatty acids may have protective effects against breakouts
- While plant-based diets offer many health advantages, their specific benefits for acne management remain inconclusive
- Probiotic foods show promise but require more research to confirm their effectiveness for acne treatment
Effective Home Remedies
While not all home treatments prove effective, several natural approaches have shown promise for managing mild acne:
Tea Tree Oil: With natural antimicrobial properties, diluted tea tree oil can help reduce inflammation when applied topically.
Aloe Vera: This plant extract offers soothing properties that may calm irritated skin and reduce redness.
Honey Masks: Raw honey contains antibacterial compounds and can serve as a gentle, natural cleanser.
Green Tea: Applied topically, green tea’s antioxidants may help reduce sebum production and inflammation.
Hands-Off Approach: Perhaps the simplest yet most important home remedy is avoiding touching your face, which transfers bacteria and oils from your hands to already vulnerable skin.
No Squeezing: Resist the urge to pop or squeeze pimples, as this can drive bacteria deeper, spread infection, and significantly increase scarring risk.
Preventing Acne
While completely preventing acne isn’t always possible, especially for those with genetic predispositions, these strategies can help minimize breakouts:
Consistent Cleansing: Wash your face daily with a gentle, oil-free cleanser to remove excess sebum without irritating skin.
Appropriate Products: Consider trying over-the-counter acne cleansers containing ingredients like salicylic acid or benzoyl peroxide for oily skin.
Makeup Choices: Select water-based, non-comedogenic cosmetics that won’t clog pores.
Evening Routine: Always remove makeup and thoroughly cleanse your skin before sleeping.
Post-Exercise Hygiene: Shower or wash your face after physical activity to remove sweat and oils.
Hair Management: Keep long hair away from your face and forehead to prevent additional oil transfer.
Clothing Considerations: Avoid tight headbands, hats, and clothing that rub against acne-prone areas, creating friction and irritation.
Lifestyle Factors: Maintain a balanced diet, stay well-hydrated, and implement stress management practices, as heightened stress levels can trigger hormonal changes that worsen acne.
When to Seek Medical Help
While mild acne can often be managed with over-the-counter treatments, you should consider consulting a dermatologist if:
- Your acne is severe or widespread
- You’re developing scars or dark spots after acne healing
- Over-the-counter products haven’t helped after several months
- Your acne is causing significant emotional distress
A dermatologist can provide prescription-strength treatments and personalized advice to help manage your acne effectively.
The Emotional Impact and Outlook
It’s important to acknowledge that acne can cause significant emotional distress, affecting self-confidence and social interactions. Remember that you’re not alone – acne affects nearly everyone at some point in their lives, and many people experience it well into adulthood.
The encouraging news is that effective treatments exist for all forms of acne. With appropriate care, you may notice improvements within weeks of beginning treatment. Seeking treatment early can also help prevent or minimize scarring.
Even with the best treatment plans, occasional flare-ups may still occur. Persistent or severe acne might require long-term management strategies. Working with a dermatologist to develop a customized treatment approach offers the best chance for clear, healthy skin.
Final Thoughts
Acne is a complex condition influenced by various factors including genetics, hormones, lifestyle, and environment. Understanding your specific triggers is the first step toward effective management. With the right approach and possibly professional guidance, most cases of acne can be successfully controlled, helping you achieve clearer, healthier skin and improved confidence.